Dunsborough Physio - Sports Rehab
 Sports Rehabilitation
Sports Rehabilitation
At Dunsborough Physiotherapy Centre we supply innovative evidence-based Sports Rehabilitation Services for those sportsmen and sportswomen who have sustained an injury during sport. Over the years at Dunsborough Physiotherapy Centre our physios have treated sportsmen and sportswomen of all standards, from Olympic athletes to casual social participants. Our Dunsborough physiotherapists have a wealth of knowledge and are able to supply effective individualised sports rehabilitation programs for injured athletes wanting to get back to what they love as soon as possible . Our physiotherapy team are all keen sporting participants involved in a number of sports locally: soccer, tennis, surfing, running, cycling, netball, swimming, triathlons........and more. Our physio staff have access to, and utilise, the latest research to provide up-to-date effective rehabilitation programs. We are also well versed in the provision of post-surgical rehabilitation and follow evidence-based post-surgical rehab protocols. If you require rehabilitation following a sporting injury or post-surgery the team of highly skilled physiotherapists at Dunsborough Physiotherapy Centre can help.
We are proud sponsors of numerous junior sports clubs in Dunsborough.
Sports Rehab for Juniors: Dunsborough Physiotherapy Centre staff are heavily involved in the management and prevention of sporting injuries in junior sportspersons. We treat many younger athletes in a wide range of sporting codes. Dunsborough Physiotherapy Centre staff have treated a number of SWAS (South West Academy of Sport) juniors over the years providing conditioning programs, injury rehabilitation and injury prevention strategies. Regardless of your skill level we are able to help you with your sports rehab requirements.
Ben Liston has introduced the SPRIG program (Stretch Pro-actively to Reduce Injury to Growth-plates) to junior sporting associations to help reduce injury rates in our junior sportspersons. Ben is heavily involved in junior sport, not only as a physiotherapist, but also as a local coach.
For more information visit our SPRIG program page: click / tap here.
Ben Liston has introduced the SPRIG program (Stretch Pro-actively to Reduce Injury to Growth-plates) to junior sporting associations to help reduce injury rates in our junior sportspersons. Ben is heavily involved in junior sport, not only as a physiotherapist, but also as a local coach.
For more information visit our SPRIG program page: click / tap here.
 Cutting-edge technology
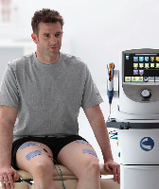
Cutting-edge technology
We have access to cutting edge technologies to aid your recovery from injury and monitor your progress accurately. Real-time ultrasound (to assess deep abdominal strength), EMG (electromyography) to assess muscle activation accurately, biofeedback devices (for assessment of appropriate muscle recruitment) laser, therapeutic ultrasound, interferential, TENS, muscle stimulation (to help stimulate the contraction of weakened musculature), dynamometry (to accurately assess muscle strength), goniometry (to assess joint ROM / flexibility), resistance devices (resistance band and resistance tubing), weights, fitballs, rollers, balance disks and wobble-boards (to challenge balance), and variable height steps are just some of the assessment and treatment tools at our disposal. We will make sure you are ready to return to the sport you love with adequate global strength, flexibility, core strength, stamina and balance (proprioception) so as to limit your risk of re-injury. We will incorporate sports-specific drills to help prepare you for your return to sport. At Dunsborough Physiotherapy Centre we provide biomechanical analysis and injury prevention strategies to limit your chance of injury during sport.
Sports Rehab Services Provided
 Hands-on treatment
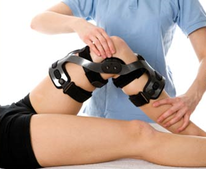
Hands-on treatment
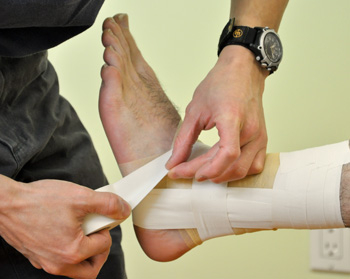
Hands-On Treatment and Home Exercise Program Provision: Dunsborough Physiotherapy staff are able to supply effective in-room hands-on treatment as part of a comprehensive sports rehab program. We can also formulate a home exercise program specific to your condition and your stage of recovery. This program will include all the necessary exercises to improve strength, flexibility, range of joint motion, and balance (proprioception). We will progress your home exercise program in accordance with your stage of recovery. Our physiotherapists will assess your biomechanics as required, to ensure that any faults in technique are recognised and altered accordingly. We use a number of hands-on physiotherapy treatment techniques to speed recovery including joint mobilisation techniques, soft tissue mobilisation, neural stretching, muscle strengthening, rigid sports taping and kinesio taping techniques, massage, dry needling, trigger point therapy and more. We have access to numerous technologies as mentioned above which we employ as part of our sport rehabilitation therapy.
 Post-Surgical Rehab
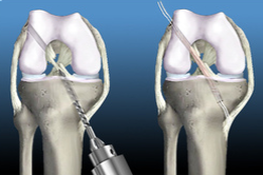
Post-Surgical Rehab
Post-surgical rehabilitation: if you have required surgical intervention following a sporting injury we are able to deliver high quality rehabilitation to speed your recovery. We are aware of the most up-to-date rehab protocols, and will supply a rehab program specific to your surgery, and your surgeon's protocols. We are able to supply hands-on treatment using treatment techniques designed to relieve pain, decrease swelling, increase movement and improve muscle strength. At Dunsborough Physiotherapy Centre we also offer one-on-one hydrotherapy, pilates, massage, and physiotherapy-supervised individually designed gym programs (incorporating strengthening, stretching, joint range of movement and proprioception exercises).
We are able to accurately monitor your progress with cutting-edge technology: goniometry to assess joint range of motion and flexibility, hand dynamometry and push/pull dynamometry to assess muscle strength, real-time ultrasound to assess core-strength and pelvic floor activation, and electromyography to assess muscle activity and strength.
We are able to accurately monitor your progress with cutting-edge technology: goniometry to assess joint range of motion and flexibility, hand dynamometry and push/pull dynamometry to assess muscle strength, real-time ultrasound to assess core-strength and pelvic floor activation, and electromyography to assess muscle activity and strength.
 Hydrotherapy
Hydrotherapy
Hydrotherapy: often a useful part of sports rehabilitation, particularly in the early phases of recovery or post-surgically, Dunsborough Physiotherapy Centre offers a one-on-one hydrotherapy service. Megan Liston, a physiotherapist with over 20 years of experience will structure a hydrotherapy rehab program specific to your needs, following the relevant post-surgical physio rehabilitation guidelines.
A water medium provides the advantages of buoyancy to de-load weight-bearing structures. The warmth of the water can aid mobility and reduce pain. The resistance of water can be useful to help strengthen weakened muscle groups. Turbulence of water can be used to challenge proprioception (balance). Megan is able to supervise your hydrotherapy program regularly and progress your exercises as appropriate to help speed your recover post-surgery.
A water medium provides the advantages of buoyancy to de-load weight-bearing structures. The warmth of the water can aid mobility and reduce pain. The resistance of water can be useful to help strengthen weakened muscle groups. Turbulence of water can be used to challenge proprioception (balance). Megan is able to supervise your hydrotherapy program regularly and progress your exercises as appropriate to help speed your recover post-surgery.
 Individualised Gym Programs
Individualised Gym Programs
Gym Programs: The physiotherapy staff at Dunsborough Physiotherapy Centre are highly skilled in the development of innovative and appropriate gym programs to aid in your recovery from injury. The physio staff can supply a gym program which is specific to your injury. Gym programs will be progressed at regular intervals to ensure a rapid return to sport. We are able to supervise your program one-on-one as often as is necessary. We will also suggest a home-based exercise program as required to target specific areas of concern. Our staff have great knowledge and background in exercise prescription and progression. We will incorporate both free weights and chain weights into your program. Importantly we will not only prescribe strengthening exercises for global muscle groups, but also ensure that adequate core strengthening is a part of your routine to lessen the risk of re-injury.
 Pilates
Pilates
Pilates: Core strengthening is an integral part of any sports rehab program. Dunsborough Physiotherapy Centre supplies one-on-one, and small group size pilates tuition. Pilates is one of the better methods of improving core strength. Evie Crowe, a physiotherapist with many years of physiotherapy experience supplies one-on-one tuition, and will progress you at an appropriate pace to ensure you engage your core effectively. A strong base of support is essential to deliver maximal global musculature power. Prescription of a home-based pilates exercise routine is also offered and is often effective in ensuring core musculature is properly engaged: often not the case if pilates exercises are progressed too rapidly. We have access to Real-Time Ultrasound to assess your deep abdominal and pelvic floor function this assessment tool will ensure you are properly engaging these core muscle groups during exercise.
Post-Injury Sports Rehab: Acute injury management (RICER)
General Injury Prevention Strategies - Sports Rehab
 General Injury Prevention
General Injury Prevention
There are a number of general injury prevention strategies which apply to all activities and sports. For more specific detail in regards to injury prevention strategies specific to your sport / activity of choice contact Dunsborough Physiotherapy Centre. Our physios can provide an exercise program to limit your risk of injury.
Injury Prevention - General Guidelines
Pre-Season Conditioning
Pre-Game Warm-Up / Stretching and Post-Game Cool-Down
Wearing of Protective Clothing
Appropriate Footwear
Balance Training
Core Strengthening
Relevant Global Musculature strengthening
Flexibilty / Joint Range of Movement program
Correct Biomechanics / Technique
Proper Nutrition: including hydration, carbohydrate intake and electrolyte intake.
Injury Prevention - General Guidelines
Pre-Season Conditioning
Pre-Game Warm-Up / Stretching and Post-Game Cool-Down
Wearing of Protective Clothing
Appropriate Footwear
Balance Training
Core Strengthening
Relevant Global Musculature strengthening
Flexibilty / Joint Range of Movement program
Correct Biomechanics / Technique
Proper Nutrition: including hydration, carbohydrate intake and electrolyte intake.
 Hamstring Stretch
Hamstring Stretch
The Rules of Stretching:
-Do not make stretches competitive.
- -Warm-up the body prior to stretching
- -Stretch before and after exercise (active stretching during the warm up, static stretching during the cool down)
- -Stretch all muscle groups that will be involved in the activity
- -Stretch gently and slowly: longer holds (20 seconds+) are better than shorter holds.
- -Never bounce or stretch rapidly
- -Stretch gently to the point of mild discomfort, never pain
-Do not make stretches competitive.
Useful Links - Sports Injury Management / Research
Dunsborough Physiotherapy Sports Rehab - Your Sports Injury
Find your sport of choice listed below and discover common injuries associated with your sport, common causes of injury, and injury prevention strategies. If you need help with your sporting injury Dunsborough Physiotherapy Centre have a wealth of knowledge in the area of sports rehab and can help.
 Surfing Injury Management
Surfing Injury Management
Surfing Injuries (short-board / long-board), Stand-Up Paddleboarding, and Body-Boarding
Ben, Harumi, Megan, and Caris are all keen surfers and are aware of the injuries commonly incurred whilst surfing. Ben Liston has surfed for over 30 years and has treated a huge number of surfers over his career including WCT (World Championship Tour) athletes. At Dunsborough Physiotherapy Centre we regularly treat surfers of all abilities suffering injuries incurred locally in the powerful surf of the southwest of W.A. The team at Dunsborough Physiotherapy Centre are able to accurately assess your surfing-related injury and supply effective treatment to speed your recovery. Whether it is post-injury or post-surgical rehabilitation required our team of physiotherapists have great experience in the assessment and treatment of surfing injuries and can help.
Common surfing injuries:
The most common surfing injuries requiring treatment are lacerations, sprains, dislocations and
fractures. The most common surfing injury is a laceration or cut, accounting for about half of all surfing injuries. Half of all lacerations are caused by direct contact with the sea floor. Joint sprains account for 1/4 of all surfing injuries, most commonly to the back, shoulder, knee, and ankle. Dislocations and fractures account for the remainder of injuries with the nose, teeth, and ribs the most common fracture sites. The legs (37%) and head (35%) are most common areas of injury. The torso (16%) and arms (12%) account for the rest of injuries. Acute injuries account for almost 75% of surfing injuries. Aside from lacerations, acute knee injuries are common: two-thirds of knee injuries are sprains, cartilage tears, and dislocations, mostly caused by excessive body torque when performing turns on the wave face, when landing from aerial manoeuvres, or due to a fall. Surfers are also prone to chronic overuse injuries. The most common chronic overuse injuries involve the shoulder, back, and neck due to repeated paddling. Chronic ligament sprains of the knee occur commonly due to frequent turns and twists.
At Dunsborough Physiotherapy Centre we most commonly see knee meniscal injuries, ACL (anterior cruciate ligament) ruptures, MCL (medial collateral ligament) sprains, ankle inversion sprains, hamstring and groin (adductor) strains, low back (disc injury / facet joint irritation), neck pain (facet joint irritation, disc injury and / or nerve root irritation), and shoulder injuries (dislocation / impingement syndrome involving the rotator cuff tendons, and sub-acromial bursa).
Common causes of surfing injuries:
The most common cause (almost 50%) of acute injury in surfers is hitting a surfboard, either your own or someone else's. Wipeouts in deeper water cause about one-third of all injuries. Falling and hitting the seafloor is responsible for almost 20% of surfing injuries. Reef seabeds double the risk of injury compared to sandy seabeds.
Who gets injured?
Experienced surfers tend to have more severe injuries than novices, most likely because they surf larger waves in more challenging conditions.
Inexperienced surfers tend to be injured more frequently, although their injuries tend to be less serious. Competitive surfers have slightly higher injury
rates than recreational surfers: 1 injury for every 150 hours of surfing. However, competitive surfers usually ride higher waves, perform numerous turns
and twists, and often execute aerial manoeuvres. Variables that increase the risk for a serious injury are: age over 30 years old, advanced or expert surfing ability, and wave size over head-high. There is no difference in the injury rates between men and women.
Injury Prevention:
Ben, Harumi, Megan, and Caris are all keen surfers and are aware of the injuries commonly incurred whilst surfing. Ben Liston has surfed for over 30 years and has treated a huge number of surfers over his career including WCT (World Championship Tour) athletes. At Dunsborough Physiotherapy Centre we regularly treat surfers of all abilities suffering injuries incurred locally in the powerful surf of the southwest of W.A. The team at Dunsborough Physiotherapy Centre are able to accurately assess your surfing-related injury and supply effective treatment to speed your recovery. Whether it is post-injury or post-surgical rehabilitation required our team of physiotherapists have great experience in the assessment and treatment of surfing injuries and can help.
Common surfing injuries:
The most common surfing injuries requiring treatment are lacerations, sprains, dislocations and
fractures. The most common surfing injury is a laceration or cut, accounting for about half of all surfing injuries. Half of all lacerations are caused by direct contact with the sea floor. Joint sprains account for 1/4 of all surfing injuries, most commonly to the back, shoulder, knee, and ankle. Dislocations and fractures account for the remainder of injuries with the nose, teeth, and ribs the most common fracture sites. The legs (37%) and head (35%) are most common areas of injury. The torso (16%) and arms (12%) account for the rest of injuries. Acute injuries account for almost 75% of surfing injuries. Aside from lacerations, acute knee injuries are common: two-thirds of knee injuries are sprains, cartilage tears, and dislocations, mostly caused by excessive body torque when performing turns on the wave face, when landing from aerial manoeuvres, or due to a fall. Surfers are also prone to chronic overuse injuries. The most common chronic overuse injuries involve the shoulder, back, and neck due to repeated paddling. Chronic ligament sprains of the knee occur commonly due to frequent turns and twists.
At Dunsborough Physiotherapy Centre we most commonly see knee meniscal injuries, ACL (anterior cruciate ligament) ruptures, MCL (medial collateral ligament) sprains, ankle inversion sprains, hamstring and groin (adductor) strains, low back (disc injury / facet joint irritation), neck pain (facet joint irritation, disc injury and / or nerve root irritation), and shoulder injuries (dislocation / impingement syndrome involving the rotator cuff tendons, and sub-acromial bursa).
Common causes of surfing injuries:
The most common cause (almost 50%) of acute injury in surfers is hitting a surfboard, either your own or someone else's. Wipeouts in deeper water cause about one-third of all injuries. Falling and hitting the seafloor is responsible for almost 20% of surfing injuries. Reef seabeds double the risk of injury compared to sandy seabeds.
Who gets injured?
Experienced surfers tend to have more severe injuries than novices, most likely because they surf larger waves in more challenging conditions.
Inexperienced surfers tend to be injured more frequently, although their injuries tend to be less serious. Competitive surfers have slightly higher injury
rates than recreational surfers: 1 injury for every 150 hours of surfing. However, competitive surfers usually ride higher waves, perform numerous turns
and twists, and often execute aerial manoeuvres. Variables that increase the risk for a serious injury are: age over 30 years old, advanced or expert surfing ability, and wave size over head-high. There is no difference in the injury rates between men and women.
Injury Prevention:
- Buy protective equipment. Use rubber guards for the nose and fins of your board to prevent lacerations. Wetsuits can also prevent lacerations from fins. Only 5% of surfers use rubber guards.
- Wear a helmet to prevent head injuries, especially when surfing near shallow reefs or in crowded conditions. Only 5% of surfers regularly wear helmets. Although concussions account for only 6% of surfing injuries, they are potentially the most serious because they can result in drowning. One out of every 100 surfers has reported a near-drowning experience. Never surf alone.
- A surfboard leash ensures access to a flotation device in case of disabling injury and lowers risk of injuries to others from loose boards. However, leash recoil increases the odds of the board striking you in the face or head.
- Good physical fitness, including strengthening and stretching the neck, shoulders, and back, can help to prevent chronic injuries. Improved proprioception may also help to lessen knee and ankle injury rates in surfers. Proper landing technique can help to lessen angulation at the knee and reduce the risk of ligament / meniscal injury. Correct paddling technique can lessen potential impingement and rotator cuff / sub-acromial bursal problems. Correct neck and head position during paddling and duck-diving can lessen stress on the neck.
- Ask the locals about water conditions before surfing in an unfamiliar area.
- Be realistic about your abilities; don't be peer-pressured to surf waves beyond your skill level.
- Stay sober. One in 100 surfers has admitted surfing while under the influence of drugs or alcohol.
- Spread out. It is typical to have 15 surfers in the water at any one time. Injury rates have been shown to increase with more surfers in the water.
Winter Team Sports Injuries
Dunsborough Physiotherapy Centre is kept busy through the winter months. We see a large number of winter sporting injuries across all sports codes, both senior and junior. Our physiotherapy team are well versed in the treatment of all sporting injuries and are able to provide effective up-to-date evidence-based rehabilitation to return you to your chosen sport as soon as possible. Below you will find some useful information in regard to common winter sporting injuries, injury risk factors relating to your specific winter sporting pursuit, and specific injury prevention strategies.
Dunsborough Physiotherapy Centre is kept busy through the winter months. We see a large number of winter sporting injuries across all sports codes, both senior and junior. Our physiotherapy team are well versed in the treatment of all sporting injuries and are able to provide effective up-to-date evidence-based rehabilitation to return you to your chosen sport as soon as possible. Below you will find some useful information in regard to common winter sporting injuries, injury risk factors relating to your specific winter sporting pursuit, and specific injury prevention strategies.
 Rugby Injuries
Rugby Injuries
Rugby Injuries: Rugby Union is a contact sport with players requiring strength, speed, agility and ball handling and kicking skills. Four body regions account for half of all Rugby Union injuries: shoulder (18%), knee (13%), thigh (12%) and ankle (12%). Sprain/strain injuries account for 58% of injuries. The tackle (52%), overexertion and overuse (14.5%) are also common. The tackle is the most frequent cause of injury (>50%). As many as 1 in 4 rugby players will be injured during a season. On average each player performs 20- 40 tackles per match. Almost 25% of neck injuries occur when there is a mismatch in experience between the two opposing front rows. Rugby injury rates are reported to be nearly three times higher than soccer. Most rugby injuries are experienced by 10-18 year olds.
When Do Rugby Injuries Occur? - More injuries occur during matches (57%) than in training, and more often in the second half of the game.
Risk factors: Hookers and flankers sustain the most injuries. Mismatched team skill levels, playing in a forward position, being tackled, and time of season (early season) are other important risk factors in rugby.
Common Injuries In Rugby:Over 40% of injuries are muscular strains or contusions (haematoma / bruising), 30% are sprains, followed by dislocations, fractures, lacerations, and overuse injuries. Sprained ankles are a common injury with ankle sprains representing almost 1 in 7 rugby injuries.
Injury prevention: Pre-Season preparation is important. More injuries occur at the beginning of a season, suggesting that pre-season conditioning could reduce injuries. A pre-season conditioning program should gradually increase in intensity and duration to prepare athletes for competition.
coaching effective defensive skills, correct tackling technique, correct falling technique and methods to minimise the absorption of impact forces in tackles can help to reduce injury rates in rugby players. To reduce scrummaging injuries at lower rugby levels, props should crouch, touch, pause and then engage. This technique is called "depowering the scrum". Another alternative is "sequential engagement" where the front rows engage first and then the second row joins in so that a stable scrum is established. Protective clothing (scrum caps, shoulder pads, shin guards and mouth guards) reduce injury in rugby players. Stretching and strengthening of relevant muscle groups, improving proprioception and correct technique when tackling can also reduce risk of injury. Taping ankles can help to reduce ankle sprain rates.
When Do Rugby Injuries Occur? - More injuries occur during matches (57%) than in training, and more often in the second half of the game.
Risk factors: Hookers and flankers sustain the most injuries. Mismatched team skill levels, playing in a forward position, being tackled, and time of season (early season) are other important risk factors in rugby.
Common Injuries In Rugby:Over 40% of injuries are muscular strains or contusions (haematoma / bruising), 30% are sprains, followed by dislocations, fractures, lacerations, and overuse injuries. Sprained ankles are a common injury with ankle sprains representing almost 1 in 7 rugby injuries.
Injury prevention: Pre-Season preparation is important. More injuries occur at the beginning of a season, suggesting that pre-season conditioning could reduce injuries. A pre-season conditioning program should gradually increase in intensity and duration to prepare athletes for competition.
coaching effective defensive skills, correct tackling technique, correct falling technique and methods to minimise the absorption of impact forces in tackles can help to reduce injury rates in rugby players. To reduce scrummaging injuries at lower rugby levels, props should crouch, touch, pause and then engage. This technique is called "depowering the scrum". Another alternative is "sequential engagement" where the front rows engage first and then the second row joins in so that a stable scrum is established. Protective clothing (scrum caps, shoulder pads, shin guards and mouth guards) reduce injury in rugby players. Stretching and strengthening of relevant muscle groups, improving proprioception and correct technique when tackling can also reduce risk of injury. Taping ankles can help to reduce ankle sprain rates.
 Hockey Injuries
Hockey Injuries
Hockey Injuries: The modern game of hockey is played in 132 countries around the world and is second only in popularity to soccer as a team sport. Hockey players are not immune to injury. Those aged 10 to 19 years account for 50% of injuries, mostly in the 15-19 year age group. Overuse injuries to the ankles and lower back are common. Acute injuries commonly affect the upper limb (mostly hand and forearm), the face, and lower limb (mostly ankle, foot and knee). Common types of injury include fractures, sprains / strains and bruising. Injury rates are higher at the start of the season. The rate of injury for community level hockey players is 15 injuries per 1,000 playing hours.
Injury Prevention: enforcing rules aimed at preventing dangerous use of the hockey stick and careless play of the ball, modifying rules for children, use of protective equipment (such as shin guards, eye wear and mouthguards), expert training of coaches and officials, adequate nutrition, pre-season conditioning, pre-game stretch and warm-up, post-game cool-down, prompt access to professional first aid and medical care, full rehabilitation before returning to play including biomechanical analysis, taping of ankles, correct footwear, core strengthening, proprioception (balance) exercises and the wearing of protective gloves are all relevant in lowering injury levels in hockey.
Injury Prevention: enforcing rules aimed at preventing dangerous use of the hockey stick and careless play of the ball, modifying rules for children, use of protective equipment (such as shin guards, eye wear and mouthguards), expert training of coaches and officials, adequate nutrition, pre-season conditioning, pre-game stretch and warm-up, post-game cool-down, prompt access to professional first aid and medical care, full rehabilitation before returning to play including biomechanical analysis, taping of ankles, correct footwear, core strengthening, proprioception (balance) exercises and the wearing of protective gloves are all relevant in lowering injury levels in hockey.
 Soccer Injuries
Soccer Injuries
Soccer Injuries: most soccer injuries affect the lower extremities and are caused by trauma, such as a collision with an opponent or landing awkwardly from a jump, though 1/4 to 1/3 of all soccer injuries are due to overuse and develop over a period of time. The rate of injury for soccer players is up to 35 injuries per 1,000 playing hours. The older the player, the more likely they are to get injured. The most common injuries in soccer are contusion (haematoma), hamstring injury, ankle sprain, meniscal (knee cartilage) injury, low back disc injury, concussion, and ACL (anterior cruciate ligament) tear. Ankle sprains are singularly the most common injury in soccer. Ankle sprains usually follow a typical pattern: occurring when the sole of the foot rolls inwards, damaging the ligaments on the outside of the ankle. Landing / running on uneven ground or landing on another player’s foot are common mechanisms of injury, as is an opponent sliding in and hitting the inside of a player's lower leg, forcing the foot to roll inwards. The knee is the second most commonly injured joint in soccer players. The most severe injury in soccer is an anterior cruciate ligament rupture. Direct injury (being tackled or receiving a blow) or indirect injury (pivoting, twisting) may affect the ligaments (particularly the anterior cruciate ligament), or the meniscal cartilage of the knee. The ACL is one of the major stabilising ligaments in the knee joint that prevents excessive movement of the lower leg in relation to the thigh. Seventy per cent of all ACL injuries occur without contact with another player. Mechanisms of ACL injury in soccer players involves a one-step stop deceleration, a sudden change of direction, landing from a jump with the knee and hip in extension, or a lapse in concentration. Hamstring injury is the most common muscular injury in soccer. Most hamstring strains occur without impact or contact with another player during sprinting or acceleration. Weakness and inflexibility in the hamstring group along wit low back pathology increases risk of injury. Other common muscle groups susceptible to injury in soccer are the quadriceps (rectus femoris), adductors (adductor longus), and the calves (particularly the gastrocnemius).
Injury prevention: balance (proprioception) improvement, landing drill practice, wearing of ankle braces / taping ankles (particularly if you have suffered a previous ankle sprain), calf stretching, evertor strengthening, hamstring strengthening and stretching, adductor stretching and strengthening, employment of the FIFA 11+ program (a warm-up injury prevention program) - click here for more info, wearing of protective clothing (shin guards, mouth guard), and wearing appropriate footwear all help to reduce injury rates in soccer players.
Injury prevention: balance (proprioception) improvement, landing drill practice, wearing of ankle braces / taping ankles (particularly if you have suffered a previous ankle sprain), calf stretching, evertor strengthening, hamstring strengthening and stretching, adductor stretching and strengthening, employment of the FIFA 11+ program (a warm-up injury prevention program) - click here for more info, wearing of protective clothing (shin guards, mouth guard), and wearing appropriate footwear all help to reduce injury rates in soccer players.
 Netball Injuries
Netball Injuries
Netball Injuries: Netball is one of the most popular team sports in Australia. The rate of injury for netballers is 14 injuries per 1,000 hours played. Adults in formal play are predominantly injured as a result of a collision (26%), while children are injured due to falling (23%). Sprains and strains are the dominant injury for both child and adult injury in formal play (42% and 56%, respectively). Lower limbs are the main body region injured in formal adult netball (62%). A higher frequency of upper limb injuries are reported in formal child netball (58%). This is likely to be a result of incorrect technique and a lack of coordination, in which the child falls and uses their outstretched hands to stop them from falling heavily onto their body. Common causes of injuries are awkward landings, slips / falls, player contact / collision, overexertion, overuse, and being hit by the ball. Ankle, wrist, hand, finger and knee injuries occur frequently. The most common types of injuries are sprains, bruising, fractures and dislocations. A recent netball study found that not warming up before a game increases the risk of injury by 48%.
Common Injuries: the most common injury in netball is a sprained ankle due to landing and pivoting movements involved in netball. A sprain is a tear (partial or full) of a ligament, and in the case of the ankle, the most commonly injured ligament is the anterior talofibular ligament. This ligament lies on the outer side of the ankle joint and is injured when the player rolls the ankle inwardly (so that the sole of the foot faces inwards).
ACL rupture: the ACL (anterior cruciate ligament) is located centrally deep within the knee joint and is vital in providing stability to the knee joint, controlling the femur (thigh bone) position in relation to the tibia. The ACL is injured in non-contact sports just as frequently as contact sports. The usual mechanism of injury for an ACL tear is a twisting movement (change of direction) when weight-bearing (especially when landing from a jump) or due to a collision, forcing the knee to bend in the wrong direction (such as when another player falls across the outside of an opponents knee). Occasionally an ACL injury may occur during a sudden deceleration when running.
Patella tendinopathy also known as "Jumpers Knee" is often seen in sports involving jumping and bounding. Netball is no exception, especially when combined with the hard concrete surface it is usually played on. Patella tendinopathy is inflammation and degeneration of the patella tendon (or ligament as it is sometimes called) which attaches the quadriceps muscles to the tibia (shin bone) due to repetitive loading.
Hamstring Strain: a hamstring strain, or pulled hamstring is a common injury across all sports including netball. The usual mechanism of a hamstring injury is running (sprinting): a short burst of speed or sudden deceleration loads the hamstring dramatically, which must control the forward movement of the lower leg (ie. oppose the powerful quadriceps muscle group).
Achilles tendinopathy: the achilles tendon is the thick tendon at the back of the lower leg which attaches the calf muscles (gastrocnemius and soleus) to the back of the heel (calcaneum). Tendinopathy is a degenerative condition which causes pain, thickening and stiffness in the tendon. Achilles injuries are not uncommon in netball and similar sports such as basketball which require the athlete to jump and bound repetitively on a hard surface.
Groin strain: the groin, or adductor muscles are commonly injured in fast paced sports requiring sudden changes of direction. The action of the groin muscles is to bring the leg towards the centre and across in front of the body. The adductors also play an important role in stabilising the pelvis during weightbearing. Hip adductor injuries occur most commonly when there is a forced push-off (side-to-side motion). High forces are developed in the adductor tendons when the athlete must shift direction suddenly. As a result, the adductor muscles contract to generate opposing forces. Less commonly the hip adductors are injured from sudden overstretching.
Rotator Cuff Injury: the rotator cuff muscles are a group of four muscles which attach to the scapula (shoulder blade) and help to stabilise the shoulder joint and produce rotatory movements. Netball involves a lot of overhead throwing, catching and shooting movements, leaving players susceptible to injuries involving one or more of the rotator cuff tendons.
Injury Prevention: appropriate playing surface, correction of flawed netball technique and effective conditioning program implementation, footwear, use of orthotics, adequate treatment and rehabilitation, correct landing technique, safe playing environments, adequate warm up, cool down and stretching routine, education and training, use of mouthguards, taping and bracing, prompt treatment of injuries and enforced codes of conduct all help to reduce injury rates in netballers. The evidence for the effectiveness of certain countermeasures such as warm-up, taping and bracing and landing technique remains equivocal. Other specific injury prevention measures include proprioception exercises, hamstring strengthening, adductor strengthening, calf stretching and strengthening, rotator cuff strengthening and specific shoulder flexibility exercises to ensure equivalent inward and outward rotation range of motion.
Common Injuries: the most common injury in netball is a sprained ankle due to landing and pivoting movements involved in netball. A sprain is a tear (partial or full) of a ligament, and in the case of the ankle, the most commonly injured ligament is the anterior talofibular ligament. This ligament lies on the outer side of the ankle joint and is injured when the player rolls the ankle inwardly (so that the sole of the foot faces inwards).
ACL rupture: the ACL (anterior cruciate ligament) is located centrally deep within the knee joint and is vital in providing stability to the knee joint, controlling the femur (thigh bone) position in relation to the tibia. The ACL is injured in non-contact sports just as frequently as contact sports. The usual mechanism of injury for an ACL tear is a twisting movement (change of direction) when weight-bearing (especially when landing from a jump) or due to a collision, forcing the knee to bend in the wrong direction (such as when another player falls across the outside of an opponents knee). Occasionally an ACL injury may occur during a sudden deceleration when running.
Patella tendinopathy also known as "Jumpers Knee" is often seen in sports involving jumping and bounding. Netball is no exception, especially when combined with the hard concrete surface it is usually played on. Patella tendinopathy is inflammation and degeneration of the patella tendon (or ligament as it is sometimes called) which attaches the quadriceps muscles to the tibia (shin bone) due to repetitive loading.
Hamstring Strain: a hamstring strain, or pulled hamstring is a common injury across all sports including netball. The usual mechanism of a hamstring injury is running (sprinting): a short burst of speed or sudden deceleration loads the hamstring dramatically, which must control the forward movement of the lower leg (ie. oppose the powerful quadriceps muscle group).
Achilles tendinopathy: the achilles tendon is the thick tendon at the back of the lower leg which attaches the calf muscles (gastrocnemius and soleus) to the back of the heel (calcaneum). Tendinopathy is a degenerative condition which causes pain, thickening and stiffness in the tendon. Achilles injuries are not uncommon in netball and similar sports such as basketball which require the athlete to jump and bound repetitively on a hard surface.
Groin strain: the groin, or adductor muscles are commonly injured in fast paced sports requiring sudden changes of direction. The action of the groin muscles is to bring the leg towards the centre and across in front of the body. The adductors also play an important role in stabilising the pelvis during weightbearing. Hip adductor injuries occur most commonly when there is a forced push-off (side-to-side motion). High forces are developed in the adductor tendons when the athlete must shift direction suddenly. As a result, the adductor muscles contract to generate opposing forces. Less commonly the hip adductors are injured from sudden overstretching.
Rotator Cuff Injury: the rotator cuff muscles are a group of four muscles which attach to the scapula (shoulder blade) and help to stabilise the shoulder joint and produce rotatory movements. Netball involves a lot of overhead throwing, catching and shooting movements, leaving players susceptible to injuries involving one or more of the rotator cuff tendons.
Injury Prevention: appropriate playing surface, correction of flawed netball technique and effective conditioning program implementation, footwear, use of orthotics, adequate treatment and rehabilitation, correct landing technique, safe playing environments, adequate warm up, cool down and stretching routine, education and training, use of mouthguards, taping and bracing, prompt treatment of injuries and enforced codes of conduct all help to reduce injury rates in netballers. The evidence for the effectiveness of certain countermeasures such as warm-up, taping and bracing and landing technique remains equivocal. Other specific injury prevention measures include proprioception exercises, hamstring strengthening, adductor strengthening, calf stretching and strengthening, rotator cuff strengthening and specific shoulder flexibility exercises to ensure equivalent inward and outward rotation range of motion.
 Footy Injuries
Footy Injuries
Footy Injuries: One of the good news stories in relation to winter sports is that recent studies have indicated that the rates of injury in junior Australian football, particularly AFL Auskick, are very low. Common causes of injuries are being tackled, hit / struck by another player, hit by the ball, and falls. Injuries are more likely to occur in the first four weeks of the playing season. Injuries to the thigh, knee, lower leg and ankle are most common. The most common injuries in footy are muscle strains (particularly hamstrings followed by adductors), joint and ligament sprains (especially ankle), haematomas and concussion. The most crippling injury in footy is ACL rupture. Overuse injuries occur frequently among higher level football players. Ankle sprains are the most common injury in football. Other common injuries in footy include neck and back injury, shoulder dislocation, AC joint injury, clavicle fractures, elbow sprains, forearm and wrist sprains and fracture, calf and quadriceps strain, hip joint injury / impingement, osteitis pubis, knee ligament / meniscal injuries, leg and foot fractures / stress fractures and quadriceps and Achilles tendinopathy.
Risk factors: quadriceps, calf, hip flexors and hamstrings inflexibility and lack of endurance, and poor hamstring / quadriceps strength ratio (weak hamstrings) increase the risk of injury in footy. Decreased hip ROM and adductor weakness are related to groin strain, as is gluteal weakness. Poor balance, poor landing technique and a lack of core strength are associated with a number of injuries in footy. Poor rotator cuff strength may increase risk of shoulder dislocation.
Injury Prevention: improving proprioception (balance), landing drills practice, hamstring, quadriceps and calf strengthening, core strengthening, increasing hip ROM, improving adductor strength / pelvic stability, wearing mouthguards and headgear to lessen the chance of concussion, and wearing thigh pads to limit haematoma incidence are all relevant injury prevention strategies for footy players.
Risk factors: quadriceps, calf, hip flexors and hamstrings inflexibility and lack of endurance, and poor hamstring / quadriceps strength ratio (weak hamstrings) increase the risk of injury in footy. Decreased hip ROM and adductor weakness are related to groin strain, as is gluteal weakness. Poor balance, poor landing technique and a lack of core strength are associated with a number of injuries in footy. Poor rotator cuff strength may increase risk of shoulder dislocation.
Injury Prevention: improving proprioception (balance), landing drills practice, hamstring, quadriceps and calf strengthening, core strengthening, increasing hip ROM, improving adductor strength / pelvic stability, wearing mouthguards and headgear to lessen the chance of concussion, and wearing thigh pads to limit haematoma incidence are all relevant injury prevention strategies for footy players.
Snow Skiing and Snowboarding Injuries
 Snowboarding and Skiing Injuries
Snowboarding and Skiing Injuries
Injury rates in Skiers / Snowboarders
Whilst on the slopes there is about a 1% chance of injury on any given day. 40% of all injuries go unreported. Snowboarders are 2-5 times more likely to suffer an injury than skiers. In both skiing and snowboarding beginners suffer almost three times more injuries than more experienced participants. One study documents 49% of injured snowboarders were beginners versus 18% of beginner skiers. In skiers the injury rate for anterior cruciate ligament (ACL) sprains has more than tripled since the late 1970s, while the incidence of every other injury has declined (modern ski boots transmit forces to the knee and contribute to making sprained knees the most common injury in alpine skiing). The incidence of ACL sprain represents 33% of all knee injuries. Teenagers suffer the highest overall rate of injury in any one age group. Women are more likely to sustain upper extremity injuries and are twice as likely to suffer an ACL sprain. Muscle strains and tendinitis are common overuse injuries seen in skiing and snowboarding.
Factors affecting Injury
Factors affecting injury include the grooming of slopes, ski instruction, safety innovations in ski areas, quality of ski equipment, snow conditions, visibility, number of skiers on the slopes, skier fatigue, and the use of alcohol and other drugs. Most injuries occur between 12 noon and 4 PM.
The most critical determinants of injury however, are skier ability, relative speed in relation to athletic proficiency, and improper adjustment or poor functioning equipment. It has been estimated that 44% of all downhill ski injuries are due to improper maintenance and adjustment of equipment. Failure of binding release occurs in 70% of lower leg fractures and serious knee injuries.
Boots: Soft boots give the snowboarder twice the risk of ankle injury compared to hard boots. "Snowboarder’s ankle," a fracture of the lateral process of the talus, is caused by forced dorsiflexion and inversion at the ankle permitted by softer boots. Hard boots place the snowboarder at risk of "boot-top" fractures of the tibia and fibula as well as doubling the risk for knee injury. Commonly snowboarders fall backward as they lose their heel-edge and suffer wrist impacts, buttock contusions, axial loading spinal compressions, and occipital head injuries.
Poles: "Skier’s thumb," a sprain of the ulnar collateral ligament of the first metacarpophalangeal joint is the most common injury of the upper extremity affecting skiers. Ski poles are implicated in 24% of shoulder dislocations- causing the arm to be externally rotated and forcibly abducted in a fall.
Wrist guards: for snowboarders, the wrist is the most common site of injury, accounting for ¼ of all injuries and ½ of all fractures. Wrist guards have been shown to be very effective in preventing wrist injuries. Falling backward is the mechanism of injury in about 75% of wrist injuries.
Mechanisms of Injury
Falling: falling is the leading cause of skiing (87%) and snowboarding (75%) injuries. Skiers most commonly fall forward while snowboarders more often fall backwards.
Jumping: Unsuccessfully landing jumps is the second most common cause of snowboarding injury. Snowboarders are injured three times more frequently jumping than are skiers.
Collisions: collisions account for 10% of all injuries but 67% of hospital admissions. Most commonly collisions involve a stationary object, but often it is another person.
Snowboarders have an increased rate of head injuries at 10% compared with skiers at 5%. Almost one quarter of snowboarding injuries occur during the person’s first experience. In one study wrist injuries predominated (41%) in the beginner group, shoulder injuries were most common (38%) in the intermediate group, and head injuries predominated (36%) in the expert group. Another study reported beginner snowboarders were most likely to injure the wrists (30%); low intermediates their knees (28%), intermediates their ankles (17%), and advanced and experts, their shoulder or clavicle (14%).
Injury Prevention
Get in shape: regular general fitness and training will help reduce risk of injury. Avoid drugs and alcohol. Do not ski / snowboard if you are sick or fatigued.
Equipment: be sure your equipment is properly maintained, repaired, or replaced. Wear protective eyewear, a helmet, and wrist guards if snowboarding. Dress properly in layers. Outer wear should be made of a fabric designed to reduce sliding.
Technique: snowboarders should fall with closed fists and try to roll into a fall, spreading the force of the fall out over the body instead of in one place. Those choosing to jump must know their landing site.
Instruction: professional and certified instructors can significantly lessen injury rates and severity.
Snow Conditions: avoid icy slopes. Do not ski alone in deep powder. Avoid crowded slopes, particularly at the end of the day.
Responsibility: ski and ride within your ability. Watch for skiers downhill. Look uphill before entering a trail. Move to the side of the trail when stopping. Use devices to help prevent runaway equipment. Observe all posted signs and warnings. Have the ability to load and unload lifts. Practice courteous ski habits. "Look before you leap": use caution when jumping and leaping on the slopes, especially in snowboard and terrain parks.
Keep safe on the slopes and have a great time in the snow.
Whilst on the slopes there is about a 1% chance of injury on any given day. 40% of all injuries go unreported. Snowboarders are 2-5 times more likely to suffer an injury than skiers. In both skiing and snowboarding beginners suffer almost three times more injuries than more experienced participants. One study documents 49% of injured snowboarders were beginners versus 18% of beginner skiers. In skiers the injury rate for anterior cruciate ligament (ACL) sprains has more than tripled since the late 1970s, while the incidence of every other injury has declined (modern ski boots transmit forces to the knee and contribute to making sprained knees the most common injury in alpine skiing). The incidence of ACL sprain represents 33% of all knee injuries. Teenagers suffer the highest overall rate of injury in any one age group. Women are more likely to sustain upper extremity injuries and are twice as likely to suffer an ACL sprain. Muscle strains and tendinitis are common overuse injuries seen in skiing and snowboarding.
Factors affecting Injury
Factors affecting injury include the grooming of slopes, ski instruction, safety innovations in ski areas, quality of ski equipment, snow conditions, visibility, number of skiers on the slopes, skier fatigue, and the use of alcohol and other drugs. Most injuries occur between 12 noon and 4 PM.
The most critical determinants of injury however, are skier ability, relative speed in relation to athletic proficiency, and improper adjustment or poor functioning equipment. It has been estimated that 44% of all downhill ski injuries are due to improper maintenance and adjustment of equipment. Failure of binding release occurs in 70% of lower leg fractures and serious knee injuries.
Boots: Soft boots give the snowboarder twice the risk of ankle injury compared to hard boots. "Snowboarder’s ankle," a fracture of the lateral process of the talus, is caused by forced dorsiflexion and inversion at the ankle permitted by softer boots. Hard boots place the snowboarder at risk of "boot-top" fractures of the tibia and fibula as well as doubling the risk for knee injury. Commonly snowboarders fall backward as they lose their heel-edge and suffer wrist impacts, buttock contusions, axial loading spinal compressions, and occipital head injuries.
Poles: "Skier’s thumb," a sprain of the ulnar collateral ligament of the first metacarpophalangeal joint is the most common injury of the upper extremity affecting skiers. Ski poles are implicated in 24% of shoulder dislocations- causing the arm to be externally rotated and forcibly abducted in a fall.
Wrist guards: for snowboarders, the wrist is the most common site of injury, accounting for ¼ of all injuries and ½ of all fractures. Wrist guards have been shown to be very effective in preventing wrist injuries. Falling backward is the mechanism of injury in about 75% of wrist injuries.
Mechanisms of Injury
Falling: falling is the leading cause of skiing (87%) and snowboarding (75%) injuries. Skiers most commonly fall forward while snowboarders more often fall backwards.
Jumping: Unsuccessfully landing jumps is the second most common cause of snowboarding injury. Snowboarders are injured three times more frequently jumping than are skiers.
Collisions: collisions account for 10% of all injuries but 67% of hospital admissions. Most commonly collisions involve a stationary object, but often it is another person.
Snowboarders have an increased rate of head injuries at 10% compared with skiers at 5%. Almost one quarter of snowboarding injuries occur during the person’s first experience. In one study wrist injuries predominated (41%) in the beginner group, shoulder injuries were most common (38%) in the intermediate group, and head injuries predominated (36%) in the expert group. Another study reported beginner snowboarders were most likely to injure the wrists (30%); low intermediates their knees (28%), intermediates their ankles (17%), and advanced and experts, their shoulder or clavicle (14%).
Injury Prevention
Get in shape: regular general fitness and training will help reduce risk of injury. Avoid drugs and alcohol. Do not ski / snowboard if you are sick or fatigued.
Equipment: be sure your equipment is properly maintained, repaired, or replaced. Wear protective eyewear, a helmet, and wrist guards if snowboarding. Dress properly in layers. Outer wear should be made of a fabric designed to reduce sliding.
Technique: snowboarders should fall with closed fists and try to roll into a fall, spreading the force of the fall out over the body instead of in one place. Those choosing to jump must know their landing site.
Instruction: professional and certified instructors can significantly lessen injury rates and severity.
Snow Conditions: avoid icy slopes. Do not ski alone in deep powder. Avoid crowded slopes, particularly at the end of the day.
Responsibility: ski and ride within your ability. Watch for skiers downhill. Look uphill before entering a trail. Move to the side of the trail when stopping. Use devices to help prevent runaway equipment. Observe all posted signs and warnings. Have the ability to load and unload lifts. Practice courteous ski habits. "Look before you leap": use caution when jumping and leaping on the slopes, especially in snowboard and terrain parks.
Keep safe on the slopes and have a great time in the snow.
Summer Team Sports and Individual Sports Injuries
At Dunsborough Physiotherapy Centre we see a large number of summer sports injuries relating to individual pursuits, team sports, and water sports. Injuries are spread across a wide age group. Our physiotherapy team are well versed in the treatment of all sporting injuries and are able to provide effective up-to-date evidence-based rehabilitation to return you to your chosen sport as soon as possible. Below you will find some useful information in regard to some of the more common summer sporting injuries, injury risk factors relating to your specific summer sporting pursuit, and sports-specific injury prevention strategies.
At Dunsborough Physiotherapy Centre we see a large number of summer sports injuries relating to individual pursuits, team sports, and water sports. Injuries are spread across a wide age group. Our physiotherapy team are well versed in the treatment of all sporting injuries and are able to provide effective up-to-date evidence-based rehabilitation to return you to your chosen sport as soon as possible. Below you will find some useful information in regard to some of the more common summer sporting injuries, injury risk factors relating to your specific summer sporting pursuit, and sports-specific injury prevention strategies.
 Cricket Injuries
Cricket Injuries
Cricket Injuries: Injuries in cricket are common, particularly to fast bowlers. These injuries are often due to overuse and tend to present gradually over time. Injury rates in fast bowlers are as high as 18%, which is significantly higher than other disciplines: batsmen (7%), spin bowlers (6%) and wicket-keepers (4%).
The most common injury in cricket is a hamstring strain. Traumatic injuries to the hands and fingers are also common, usually as a result of impact with the ball when fielding, wicket-keeping or batting. Throwing injuries, such as rotator cuff tendinopathy and SLAP lesions are also commonly seen.
Injuries to batsmen in cricket are common. Batting involves rapid acceleration, deceleration and sudden changes in direction when running between the wickets. As a result, muscle tears and strains are common in the lower limbs (calf and hamstring). Sudden changes in direction can also cause injuries to the ankle and knee (ankle sprain / meniscal injury). The stooped batting posture can lead to lower back pain- caused by lumbar disc degeneration. Pain in the elbow and forearm following repetitive or prolonged gripping of the bat is typically due to tennis elbow. Often the grip size may be inappropriate, the bat too heavy, or the batting technique flawed. The other common type of injuries sustained by batsmen are traumatic fractures to the hand and fingers from the ball forcefully hitting the gloves: metacarpals or phalanges tend to be the most commonly affected bones.
Injuries to bowlers in cricket are common, with fast bowling being the most injury prone discipline in the sport. Bowling, particularly fast bowling, places a large strain on the lower back. A force of 8-10 times body weight is transmitted through the body at front foot landing of the delivery stride. This, combined with extremes of lumbar range of movement, including extension, rotation and lateral flexion, puts the lumbar spine at risk of injury. Due to the repetitive nature of bowling, injuries in bowlers tend to be overuse and often present gradually over time. In younger fast bowlers (under the age of 25), lumbar stress fractures are the most prevalent injury. These injuries tend to occur on the non-bowling arm side of the lower back and are typically due to technique errors (such as a 'mixed bowling action' or excessive 'counter rotation') and/or excessive bowling workloads. In the older fast bowler degenerative lumbar injuries tend to occur more commonly, usually affecting the lumbar discs. Other common injuries to affect fast bowlers are side strains (of the non-bowling arm side of the body), posterior ankle impingement (of the front foot) and patellar tendinopathy (of the front knee). Muscle injuries to the hamstrings and groin are also frequently seen.
Wicket keeping injuries: knee pain from repetitive squatting and jumping is often the result of patellar tendinopathy, patellofemoral pain syndrome or a meniscal tear. Awkward landings from diving for balls can put the shoulder at risk of injury with shoulder impingement or rotator cuff tear a common occurrence. Groin strains often result from the side to side movement that occurs when receiving deliveries.
Fielding injuries: sudden changes in direction to field a ball can result in groin strains, meniscal injury or ankle sprains. The rapid acceleration / deceleration whilst chasing a ball can result in hamstring strains or calf strains. Throwing, or landing awkwardly from dives can result in shoulder injuries, whilst mistimed catches or awkward ground balls can result in hand or finger injuries.
Throwing Injuries: are typically due to overuse, presenting gradually overtime and often associated with poor throwing technique. Throwing injuries tend to occur in the upper limb of the throwing arm, with pain most commonly occurring in the shoulder or elbow. Common injuries include rotator cuff injuries, SLAP lesions, medial collateral ligament injury of the elbow and 1st rib stress fracture.
Injury Prevention:
- Appropriate equipment: protective equipment such as helmets, gloves, thigh pads, pads, elbow guards, a box, and shin guards help to lessen injuries related to direct impact from the cricket ball. Grip size of the bat handle- incorrect handle thickness can lead to over-gripping: a common cause of tennis elbow (tendinosis / tendinopathy of the extensor carpi radialis brevis).
- Correct technique: both for bowlers, batters and fielders correct technique is critical. Poor technique in bowlers can lead to low back stress fractures. Poor landing technique whilst bowling can lead to posterior ankle impingement. Stooped posture whilst batting can create disc-related back pain. Over-gripping of the bat handle can lead to tennis elbow.
- Appropriate workloads: in fast bowlers in particular heavy workloads can lead to chronic injury such as low back stress fracture. Rest days are essential. A slow build-up in workload is important to lessen the risk of chronic injury.
- Adequate muscle strength and flexibility: lower limb strength and flexibility is important in lessening muscle strain and tendinopathy: important muscle groups to focus on in regard to strength training in cricketers include the adductors, quadriceps, hamstrings and calves. Adequate rotator cuff strength and even amounts of inward and outward rotatory flexibility around the shoulder are important in bowlers and fielders to lessen SLAP lesions and rotator cuff pathology. Forearm strength in batters is important to lessen the chance of developing tennis elbow.
The most common injury in cricket is a hamstring strain. Traumatic injuries to the hands and fingers are also common, usually as a result of impact with the ball when fielding, wicket-keeping or batting. Throwing injuries, such as rotator cuff tendinopathy and SLAP lesions are also commonly seen.
Injuries to batsmen in cricket are common. Batting involves rapid acceleration, deceleration and sudden changes in direction when running between the wickets. As a result, muscle tears and strains are common in the lower limbs (calf and hamstring). Sudden changes in direction can also cause injuries to the ankle and knee (ankle sprain / meniscal injury). The stooped batting posture can lead to lower back pain- caused by lumbar disc degeneration. Pain in the elbow and forearm following repetitive or prolonged gripping of the bat is typically due to tennis elbow. Often the grip size may be inappropriate, the bat too heavy, or the batting technique flawed. The other common type of injuries sustained by batsmen are traumatic fractures to the hand and fingers from the ball forcefully hitting the gloves: metacarpals or phalanges tend to be the most commonly affected bones.
Injuries to bowlers in cricket are common, with fast bowling being the most injury prone discipline in the sport. Bowling, particularly fast bowling, places a large strain on the lower back. A force of 8-10 times body weight is transmitted through the body at front foot landing of the delivery stride. This, combined with extremes of lumbar range of movement, including extension, rotation and lateral flexion, puts the lumbar spine at risk of injury. Due to the repetitive nature of bowling, injuries in bowlers tend to be overuse and often present gradually over time. In younger fast bowlers (under the age of 25), lumbar stress fractures are the most prevalent injury. These injuries tend to occur on the non-bowling arm side of the lower back and are typically due to technique errors (such as a 'mixed bowling action' or excessive 'counter rotation') and/or excessive bowling workloads. In the older fast bowler degenerative lumbar injuries tend to occur more commonly, usually affecting the lumbar discs. Other common injuries to affect fast bowlers are side strains (of the non-bowling arm side of the body), posterior ankle impingement (of the front foot) and patellar tendinopathy (of the front knee). Muscle injuries to the hamstrings and groin are also frequently seen.
Wicket keeping injuries: knee pain from repetitive squatting and jumping is often the result of patellar tendinopathy, patellofemoral pain syndrome or a meniscal tear. Awkward landings from diving for balls can put the shoulder at risk of injury with shoulder impingement or rotator cuff tear a common occurrence. Groin strains often result from the side to side movement that occurs when receiving deliveries.
Fielding injuries: sudden changes in direction to field a ball can result in groin strains, meniscal injury or ankle sprains. The rapid acceleration / deceleration whilst chasing a ball can result in hamstring strains or calf strains. Throwing, or landing awkwardly from dives can result in shoulder injuries, whilst mistimed catches or awkward ground balls can result in hand or finger injuries.
Throwing Injuries: are typically due to overuse, presenting gradually overtime and often associated with poor throwing technique. Throwing injuries tend to occur in the upper limb of the throwing arm, with pain most commonly occurring in the shoulder or elbow. Common injuries include rotator cuff injuries, SLAP lesions, medial collateral ligament injury of the elbow and 1st rib stress fracture.
Injury Prevention:
- Appropriate equipment: protective equipment such as helmets, gloves, thigh pads, pads, elbow guards, a box, and shin guards help to lessen injuries related to direct impact from the cricket ball. Grip size of the bat handle- incorrect handle thickness can lead to over-gripping: a common cause of tennis elbow (tendinosis / tendinopathy of the extensor carpi radialis brevis).
- Correct technique: both for bowlers, batters and fielders correct technique is critical. Poor technique in bowlers can lead to low back stress fractures. Poor landing technique whilst bowling can lead to posterior ankle impingement. Stooped posture whilst batting can create disc-related back pain. Over-gripping of the bat handle can lead to tennis elbow.
- Appropriate workloads: in fast bowlers in particular heavy workloads can lead to chronic injury such as low back stress fracture. Rest days are essential. A slow build-up in workload is important to lessen the risk of chronic injury.
- Adequate muscle strength and flexibility: lower limb strength and flexibility is important in lessening muscle strain and tendinopathy: important muscle groups to focus on in regard to strength training in cricketers include the adductors, quadriceps, hamstrings and calves. Adequate rotator cuff strength and even amounts of inward and outward rotatory flexibility around the shoulder are important in bowlers and fielders to lessen SLAP lesions and rotator cuff pathology. Forearm strength in batters is important to lessen the chance of developing tennis elbow.
 Basketball Injuries
Basketball Injuries
Basketball Injuries
Basketball injuries are commonly caused by falls, player contact, awkward landings, sudden changes in direction and being hit by the ball. Ankle and foot injuries (sprains and fractures) are the most common injuries seen in basketball accounting for about 37% of injuries. Hip, thigh and leg injuries account for around 15% of injuries, followed by knee (ACL, PCL, LCL, or MCL ligament sprain, meniscal tear) injuries (10%-13%), forearm and wrist injuries (11%) and face / scalp (9%-12%). Shoulder injury is also common (dislocations and instability issues accounting for most occurrences). Concussion are not uncommon in basketball and depending on the grade (1,2,or 3) are managed quite differently. Hand and wrist injuries involve joint sprains and dislocations, tendon injuries and fractures.
Common overuse injuries include Jumper's knee (patellar tendinitis), plantar fasciitis, Achilles tendinitis, shin splints, and stress fractures.
Injury Prevention: wear appropriate footwear with good grip and arch support, wear ankle braces / learn to tape pre-game and pre-training, wear protective equipment (mouth-guard, safety glasses, knee and elbow pads), improve proprioception (balance) to protect knees and ankles, strengthen and stretch lower limb muscle groups, improve rotator cuff strength and scapular stabiliser strength around the shoulder, improve quadriceps / calf strength. Stretch calf muscles (gastrocnemius and soleus), practise landing drills and stay hydrated .
Basketball injuries are commonly caused by falls, player contact, awkward landings, sudden changes in direction and being hit by the ball. Ankle and foot injuries (sprains and fractures) are the most common injuries seen in basketball accounting for about 37% of injuries. Hip, thigh and leg injuries account for around 15% of injuries, followed by knee (ACL, PCL, LCL, or MCL ligament sprain, meniscal tear) injuries (10%-13%), forearm and wrist injuries (11%) and face / scalp (9%-12%). Shoulder injury is also common (dislocations and instability issues accounting for most occurrences). Concussion are not uncommon in basketball and depending on the grade (1,2,or 3) are managed quite differently. Hand and wrist injuries involve joint sprains and dislocations, tendon injuries and fractures.
Common overuse injuries include Jumper's knee (patellar tendinitis), plantar fasciitis, Achilles tendinitis, shin splints, and stress fractures.
Injury Prevention: wear appropriate footwear with good grip and arch support, wear ankle braces / learn to tape pre-game and pre-training, wear protective equipment (mouth-guard, safety glasses, knee and elbow pads), improve proprioception (balance) to protect knees and ankles, strengthen and stretch lower limb muscle groups, improve rotator cuff strength and scapular stabiliser strength around the shoulder, improve quadriceps / calf strength. Stretch calf muscles (gastrocnemius and soleus), practise landing drills and stay hydrated .
 Tennis Injuries
Tennis Injuries
Tennis Injuries: Tennis is a global sport played in more than 200 countries. Though there is much overlap with other sports in regard to injuries incurred, tennis does have its own unique injury profile. 0.04-3 injuries are incurred by tennis players per 1000 hours of play.
Common tennis injuries: injuries in tennis players are most commonly seen in the upper limb (predominantly chronic injuries) followed by the lower limb (predominantly acute injuries) and then the trunk. Some of the more common upper limb injuries are stress fractures affecting the metacarpals, hamate, radius, ulna and humerus. Tennis elbow is also very common with 9-35% of tennis players suffering from this condition at some point in their career. Risk factors for shoulder injury include a loss of internal rotation range of movement and an imbalance in external / internal rotation strength. Lower limb injuries commonly seen include tendon injuries (quadricepss, achilles, adductors), plantar fasciitis, muscle tears (most commonly calf), stress fractures and intra-articular knee injuries. Stable footwear appears important in reducing injury in the lower limb. At Dunsborough Physiotherapy Centre we commonly see a large number of tennis injuries each year including rotator cuff tears, lateral epicondylitis (tennis elbow), patello-femoral pain, meniscal tears, ACL ruptures, gastrocnemius (calf) tears, achilles tendinitis, plantar fasciitis, and low back pain relating to disc / facetal pathology. These conditions appear to be more common in the older athlete.
Injury Prevention: Correct grip size is important in reducing tennis elbow rates- the circumference of the racquet handle should be equivalent to the distance from the tip of your third finger to the proximal wrist crease. You should be able to fit the index finger of your non-hitting hand in the space between your ring finger and palm whilst gripping the racquet handle. Improving calf flexibility and strength can lessen calf tears, plantar fasciitis and achilles tendinitis. Correct biomechanics can lessen a number of tennis-related injuries. Landing drills can lessen knee and ankle injury. Double-handed back hand / correct forearm positioning during the backhand swing can lessen tennis elbow incidence. Correct serving action can lessen low back pain and injury. Improving rotator cuff / scapular stabiliser strength along with improved shoulder inward rotation range of movement can lessen shoulder injury rates . Appropriate footwear / arch support can lessen ankle sprain, calf injury and plantar fasciitis.
Improving core strength (deep abdominals) and gluteal strength (pelvic stabilisers) is also important in lessening injury rates in tennis players.
Other racquet sports: rates of injury in squash players is the highest of all racquet sports and probably relates to higher physical stress and risk of contact in this sport. Squash injuries predominantly occur in persons over 25 years (59%) i.e. the reverse for sport in general. Acute traumatic injuries are seen especially in squash players, a majority affecting the knee, lumbar region, muscles of the lower limb, and the ankle. The badminton injury pattern is similar to that of tennis and squash. Lower limb injuries predominate in all three disciplines. Most injuries affect new, infrequent, social players. Poor warm-up is a common factor in new and established players sustaining an injury.
Common tennis injuries: injuries in tennis players are most commonly seen in the upper limb (predominantly chronic injuries) followed by the lower limb (predominantly acute injuries) and then the trunk. Some of the more common upper limb injuries are stress fractures affecting the metacarpals, hamate, radius, ulna and humerus. Tennis elbow is also very common with 9-35% of tennis players suffering from this condition at some point in their career. Risk factors for shoulder injury include a loss of internal rotation range of movement and an imbalance in external / internal rotation strength. Lower limb injuries commonly seen include tendon injuries (quadricepss, achilles, adductors), plantar fasciitis, muscle tears (most commonly calf), stress fractures and intra-articular knee injuries. Stable footwear appears important in reducing injury in the lower limb. At Dunsborough Physiotherapy Centre we commonly see a large number of tennis injuries each year including rotator cuff tears, lateral epicondylitis (tennis elbow), patello-femoral pain, meniscal tears, ACL ruptures, gastrocnemius (calf) tears, achilles tendinitis, plantar fasciitis, and low back pain relating to disc / facetal pathology. These conditions appear to be more common in the older athlete.
Injury Prevention: Correct grip size is important in reducing tennis elbow rates- the circumference of the racquet handle should be equivalent to the distance from the tip of your third finger to the proximal wrist crease. You should be able to fit the index finger of your non-hitting hand in the space between your ring finger and palm whilst gripping the racquet handle. Improving calf flexibility and strength can lessen calf tears, plantar fasciitis and achilles tendinitis. Correct biomechanics can lessen a number of tennis-related injuries. Landing drills can lessen knee and ankle injury. Double-handed back hand / correct forearm positioning during the backhand swing can lessen tennis elbow incidence. Correct serving action can lessen low back pain and injury. Improving rotator cuff / scapular stabiliser strength along with improved shoulder inward rotation range of movement can lessen shoulder injury rates . Appropriate footwear / arch support can lessen ankle sprain, calf injury and plantar fasciitis.
Improving core strength (deep abdominals) and gluteal strength (pelvic stabilisers) is also important in lessening injury rates in tennis players.
Other racquet sports: rates of injury in squash players is the highest of all racquet sports and probably relates to higher physical stress and risk of contact in this sport. Squash injuries predominantly occur in persons over 25 years (59%) i.e. the reverse for sport in general. Acute traumatic injuries are seen especially in squash players, a majority affecting the knee, lumbar region, muscles of the lower limb, and the ankle. The badminton injury pattern is similar to that of tennis and squash. Lower limb injuries predominate in all three disciplines. Most injuries affect new, infrequent, social players. Poor warm-up is a common factor in new and established players sustaining an injury.
 Walking Injuries
Walking Injuries
Walking Injuries
With access to some inspiring walk paths and stunning scenery, walking is a great option in and around Dunsborough. Walking helps to maintain bone density, reduce the risk of type 2 diabetes, reduce heart disease risk / heart attack, decrease high blood pressure, improve muscle condition and create a certain level of general conditioning and aerobic fitness. Studies show that walking can reduce the risk of breast cancer and colon cancer, alleviate the symptoms of depression, and improve cognitive function. Though walking is relatively low impact the repetitive nature of walking can lead to injury. There are a number of conditions which can develop with walking. There is an overlap with running in regard to types of injuries seen.
Injuries commonly seen in walkers include:
Low back pain (disc-related / facetal), in part related to poor core strength / pelvic stability, is more common in older walkers due to degenerative changes in the lumbar spine.
Trochanteric (hip) bursitis creates pain on the outer side of the hip due to pelvic instability / iliotibial band tightness.
Retropatellar (back surface of kneecap) pain relates to poor patellar tracking, increased patello-femoral compression, and chondral wear of the retropatellar surface of the kneecap and the corresponding patellar surface of the femur.
Shin splints (medial border of shin pain) is due to a flattened or rigid foot arch, walking on hard surfaces, calf inflexibility / lack of endurance and overtraining.
Achilles tendinitis (more appropriately titled Achilles tendinosis / tendinopathy) is a condition involving degeneration / microtearing of the Achilles tendon due to repetitive loading.
Plantar fasciitis- undersurface of heel pain due to degeneration of the plantar fascia: risk factors include calf and achilles inflexibility, foot overpronation, 1st MTP inflexibility and poor footwear.
Morton's neuralgia- pain, swelling and thickening between the metatarsal heads, with potential numbness, tingling, and lancinating pain running into the toes due to a flattened transverse arch of the foot / tight footwear.
Bunions (hallux valgus)- increased angulation of the 1st MTP joint in part relating to foot overpronation.
Injury Prevention: If you are embarking on a fitness campaign which involves regular walking ensure that you increase your activity slowly. Stay on flat surfaces initially and then progress onto slopes and uneven ground. Incorporating a stretching routine can be beneficial. This should include low back range of movement exercises, stretches for the ITB and gluteals, calf stretches (gastrocnemius and soleus), quadriceps stretches, and stretches for the joints at the base of the toes. Appropriate footwear and adequate arch support is also critical. Core strengthening, gluteal strengthening (gluteus maximus, medius and minimus), quad and calf strengthening may also help to lessen injury rates in walkers.
With access to some inspiring walk paths and stunning scenery, walking is a great option in and around Dunsborough. Walking helps to maintain bone density, reduce the risk of type 2 diabetes, reduce heart disease risk / heart attack, decrease high blood pressure, improve muscle condition and create a certain level of general conditioning and aerobic fitness. Studies show that walking can reduce the risk of breast cancer and colon cancer, alleviate the symptoms of depression, and improve cognitive function. Though walking is relatively low impact the repetitive nature of walking can lead to injury. There are a number of conditions which can develop with walking. There is an overlap with running in regard to types of injuries seen.
Injuries commonly seen in walkers include:
Low back pain (disc-related / facetal), in part related to poor core strength / pelvic stability, is more common in older walkers due to degenerative changes in the lumbar spine.
Trochanteric (hip) bursitis creates pain on the outer side of the hip due to pelvic instability / iliotibial band tightness.
Retropatellar (back surface of kneecap) pain relates to poor patellar tracking, increased patello-femoral compression, and chondral wear of the retropatellar surface of the kneecap and the corresponding patellar surface of the femur.
Shin splints (medial border of shin pain) is due to a flattened or rigid foot arch, walking on hard surfaces, calf inflexibility / lack of endurance and overtraining.
Achilles tendinitis (more appropriately titled Achilles tendinosis / tendinopathy) is a condition involving degeneration / microtearing of the Achilles tendon due to repetitive loading.
Plantar fasciitis- undersurface of heel pain due to degeneration of the plantar fascia: risk factors include calf and achilles inflexibility, foot overpronation, 1st MTP inflexibility and poor footwear.
Morton's neuralgia- pain, swelling and thickening between the metatarsal heads, with potential numbness, tingling, and lancinating pain running into the toes due to a flattened transverse arch of the foot / tight footwear.
Bunions (hallux valgus)- increased angulation of the 1st MTP joint in part relating to foot overpronation.
Injury Prevention: If you are embarking on a fitness campaign which involves regular walking ensure that you increase your activity slowly. Stay on flat surfaces initially and then progress onto slopes and uneven ground. Incorporating a stretching routine can be beneficial. This should include low back range of movement exercises, stretches for the ITB and gluteals, calf stretches (gastrocnemius and soleus), quadriceps stretches, and stretches for the joints at the base of the toes. Appropriate footwear and adequate arch support is also critical. Core strengthening, gluteal strengthening (gluteus maximus, medius and minimus), quad and calf strengthening may also help to lessen injury rates in walkers.
 Running Injuries
Running Injuries
Running Injuries
Running is one of the most popular leisure sport activities. The overall yearly incidence rate for running injuries varies between 37% and 56% depending on running frequency, with 2.5 to 12.1 injuries incurred per 1000 hours of running. Most running injuries are lower extremity injuries, with knee injuries being the most common. About 50% to 75% of all running injuries appear to be overuse injuries due to constant repetition of movement. Recurrence of running injuries is reported in 20% to 70% of cases. Risk factors for running injuries include previous injury, lack of running experience, running to compete and excessive weekly running distance.
Some of the more common running injuries are documented below:
Retro-patellar pain (knee-cap pain): about 40 percent of running injuries are knee injuries. Patello-femoral pain syndrome (PFPS) typically flares up during or after long runs, after extended periods of sitting, or while descending hills and stairs. Increased compression behind the knee-cap, poor patellar tracking and chondral degradation are some of the causes of this condition.
Achilles tendinitis: (Achilles tendinosis / tendonopathy) makes up 11 percent of all running injuries. This is due to a denaturing of the Achilles tendon caused by overloading. If the tendon continues to be stressed microtears develop.
Hamstring soreness: pain felt in the back of the thigh may be due to weakness in the hamstring group, tightness, or lower back pain referral.
Calf tear: the gastrocnemius and soleus are the two major calf muscles. Tightness or lack of calf endurance / poor footwear may lead to calf tearing in the runner.
Plantar fasciitis: 15% of running injuries involve the foot. Plantar fasciitis is characterised by pain (ache) typically felt in the under-surface of the heel / arch of the foot, and is usually worse in the morning. The plantar fascia is a tough broad banded ligament-like structure running from the calcaneum (heel bone) to the bases of the toes. Poor arch support, tight calves and achilles tendon, loss of 1st MTP joint extension range of movement, and overtraining are some of the causes of this problem.
Shin splints: makes up about 15 percent of running injuries. Also known as medial tibial stress syndrome, this condition relates to irritation of the periosteum (sheath around the bone) at the site of the soleus attachment point. Poor calf endurance, poor calf flexibility, running on hard surfaces, overtraining and lack of arch support may relate to this problem.
ITBFS: Iliotibial Band Friction Syndrome (ITBFS) makes up 12 percent of all running injuries. This condition is due to the iliotibial band rubbing on the lateral epicondyle of the femur (thigh bone) due to ITB tightness and weakness in the pelvic stabilisers (gluteus medius and gluteus minimus). This condition is worsened when running on cambered surfaces, or striking on the outer aspect of the foot. It is more commonly seen in joggers compared to sprinters due to the varying amount of knee bend required in these running disciplines.
Stress fracture: stress fractures develop as a result of cumulative strain on the bone. Runners most often develop stress fractures in the tibia (shin), metatarsals (feet), or calcaneum (heel). They are one of the most serious of all running injuries.
Low back pain: in general, running does not cause lower back problems but may exacerbate existing conditions. Tight hamstrings and hip flexors may increase the risk of low back pain in runners. Common anatomical causes of back pain in runners are disc degeneration and facet joint degeneration. Improved core strength may lessen the risk of back pain whilst running.
Injury Prevention:
Adequate Recovery: allow for days off. Novice runners will need more rest days than seasoned runners.
Strength Training: improving the endurance of deep abdominals, gluteals, hamstrings, quadriceps, calves via strengthening exercises reduces injury in runners.
Stretching: stretching of appropriate muscle groups may prevent certain injuries such as retropatellar pain, achilles tendinosis, calf tear, plantar fasciitis, shin splints, ITBFS, and low back pain.
10% Rule: increase your running distance by no more than 10% per week.
Interval Training: this form of training can improve your VO2 and anaerobic threshold allowing your body to adapt to running at greater speeds without creating injury.
Warm-up and Cool-down: warm-up prepares the body for activity, as well as helping to prevent muscle injuries which can be more susceptible when cold. The cool-down helps the body clear lactic acid that builds up during any activity. Less lactic acid means less post-exercise soreness and stiffness.
Use proper equipment: appropriate footwear which absorbs shock effectively, and supports the arches of the feet appropriately is preferable. Know your foot type and buy the appropriately "lasted" shoe: speak to one of our physiotherapists for specifics.
Stay hydrated: performance begins to decrease after only a two percent loss in body water. Include electrolytes to eliminate the risk of hyponatremia if engaging in activity for more than four hours.
Consume food and drink post-exercise: the goal of post-exercise nutrition is to restore muscle and liver glycogen stores, and improve hydration. You should eat 15 to 30 minutes after exercise. Combine carbohydrates and protein together in a ratio of 4 to 1.
Running is one of the most popular leisure sport activities. The overall yearly incidence rate for running injuries varies between 37% and 56% depending on running frequency, with 2.5 to 12.1 injuries incurred per 1000 hours of running. Most running injuries are lower extremity injuries, with knee injuries being the most common. About 50% to 75% of all running injuries appear to be overuse injuries due to constant repetition of movement. Recurrence of running injuries is reported in 20% to 70% of cases. Risk factors for running injuries include previous injury, lack of running experience, running to compete and excessive weekly running distance.
Some of the more common running injuries are documented below:
Retro-patellar pain (knee-cap pain): about 40 percent of running injuries are knee injuries. Patello-femoral pain syndrome (PFPS) typically flares up during or after long runs, after extended periods of sitting, or while descending hills and stairs. Increased compression behind the knee-cap, poor patellar tracking and chondral degradation are some of the causes of this condition.
Achilles tendinitis: (Achilles tendinosis / tendonopathy) makes up 11 percent of all running injuries. This is due to a denaturing of the Achilles tendon caused by overloading. If the tendon continues to be stressed microtears develop.
Hamstring soreness: pain felt in the back of the thigh may be due to weakness in the hamstring group, tightness, or lower back pain referral.
Calf tear: the gastrocnemius and soleus are the two major calf muscles. Tightness or lack of calf endurance / poor footwear may lead to calf tearing in the runner.
Plantar fasciitis: 15% of running injuries involve the foot. Plantar fasciitis is characterised by pain (ache) typically felt in the under-surface of the heel / arch of the foot, and is usually worse in the morning. The plantar fascia is a tough broad banded ligament-like structure running from the calcaneum (heel bone) to the bases of the toes. Poor arch support, tight calves and achilles tendon, loss of 1st MTP joint extension range of movement, and overtraining are some of the causes of this problem.
Shin splints: makes up about 15 percent of running injuries. Also known as medial tibial stress syndrome, this condition relates to irritation of the periosteum (sheath around the bone) at the site of the soleus attachment point. Poor calf endurance, poor calf flexibility, running on hard surfaces, overtraining and lack of arch support may relate to this problem.
ITBFS: Iliotibial Band Friction Syndrome (ITBFS) makes up 12 percent of all running injuries. This condition is due to the iliotibial band rubbing on the lateral epicondyle of the femur (thigh bone) due to ITB tightness and weakness in the pelvic stabilisers (gluteus medius and gluteus minimus). This condition is worsened when running on cambered surfaces, or striking on the outer aspect of the foot. It is more commonly seen in joggers compared to sprinters due to the varying amount of knee bend required in these running disciplines.
Stress fracture: stress fractures develop as a result of cumulative strain on the bone. Runners most often develop stress fractures in the tibia (shin), metatarsals (feet), or calcaneum (heel). They are one of the most serious of all running injuries.
Low back pain: in general, running does not cause lower back problems but may exacerbate existing conditions. Tight hamstrings and hip flexors may increase the risk of low back pain in runners. Common anatomical causes of back pain in runners are disc degeneration and facet joint degeneration. Improved core strength may lessen the risk of back pain whilst running.
Injury Prevention:
Adequate Recovery: allow for days off. Novice runners will need more rest days than seasoned runners.
Strength Training: improving the endurance of deep abdominals, gluteals, hamstrings, quadriceps, calves via strengthening exercises reduces injury in runners.
Stretching: stretching of appropriate muscle groups may prevent certain injuries such as retropatellar pain, achilles tendinosis, calf tear, plantar fasciitis, shin splints, ITBFS, and low back pain.
10% Rule: increase your running distance by no more than 10% per week.
Interval Training: this form of training can improve your VO2 and anaerobic threshold allowing your body to adapt to running at greater speeds without creating injury.
Warm-up and Cool-down: warm-up prepares the body for activity, as well as helping to prevent muscle injuries which can be more susceptible when cold. The cool-down helps the body clear lactic acid that builds up during any activity. Less lactic acid means less post-exercise soreness and stiffness.
Use proper equipment: appropriate footwear which absorbs shock effectively, and supports the arches of the feet appropriately is preferable. Know your foot type and buy the appropriately "lasted" shoe: speak to one of our physiotherapists for specifics.
Stay hydrated: performance begins to decrease after only a two percent loss in body water. Include electrolytes to eliminate the risk of hyponatremia if engaging in activity for more than four hours.
Consume food and drink post-exercise: the goal of post-exercise nutrition is to restore muscle and liver glycogen stores, and improve hydration. You should eat 15 to 30 minutes after exercise. Combine carbohydrates and protein together in a ratio of 4 to 1.
 Swimming Injuries
Swimming Injuries
Swimming Injuries
Swimming is enjoyed by both young athletes and older age groups. The more recent popularity of triathlons and adventure sports has encouraged the older athlete to extend their "career" in the discipline of swimming. Most swimming injuries are classed as overuse injuries and relate to faulty biomechanics. Swimming has a distinct profile of injuries. Common problems seen among swimmers include "swimmer's shoulder", an overuse injury that causes inflammation of the supraspinatus tendon, sub-acromial bursa, and/or the biceps tendon, overuse injuries of the elbow (golfer's / tennis elbow), knee injuries (including breastroker's knee), ankle injuries (often tenosynovitis / tendinitis), and back injuries (stress fracture / degenerative).
Common injuries in swimmers include:-
Neck pain: more commonly seen in the older athlete, neck pain is often due to facet joint arthritic change, and disc degeneration +/- nerve root irritation. Muscle innervation and sensation to the shoulder region is predominantly derived from the C5/C6 nerve roots. If these nerve root are irritated due to degenerative change in the neck, shoulder complaints can arise. Arthritic change may also limit neck rotation making correct breathing patterns difficult. Swimmers who do not bilateral breath are more prone to neck pain. Looking forward rather than directly downward, and lifting the head too high when taking a breath can increase load on the neck and create pain.
Swimmer's Shoulder: shoulder injuries are the most common injuries seen in swimmers. "Swimmer's shoulder" is a chronic condition involving repetitive impingement of soft tissue under the coraco-acromial arch. Poor technique plays a huge role in this condition which can lead to sub-acromial bursitis, rotator cuff pathology, and long head of biceps irritation. Other shoulder problems in swimmers often relate to instability of the shoulder due to joint capsule laxity and labral (gleno-humeral gasket) damage, caused by repetitive forces placed on the anterior structures of the shoulder joint.
Breastroker's knee: this overuse condition often seen in breastrokers, involves sprain to the medial collateral ligament (MCL) due to repetitive rotatory / valgus force applied to the knee during the breastroke kick action. Poor technique is implicated in this condition.
Low Back Pain: Hyperextension of the lumbar spine during freestyle and butterfly can create low back pain, as can poor kick technique. In the younger athlete stress fractures are more common, whereas in the older athlete discal degeneration and facet joint degeneration are more common.
Biomechanical flaws: Shoulder Injury Prevention
There are a number of biomechanical flaws in a swimming stroke action which can lead to shoulder pain. Below are some of the more common shoulder issues associated with poor technique, and ways to alter your technique to lessen your chance of injury.
If pain is felt at the beginning of the freestyle stroke or as the arm starts pulling through, this may be due to the upper-arm being positioned behind the back (from shoulder to shoulder): this can cause pain. Swimmers need to be aware their arm position at the start of the stroke: the upper-arm and back have to line up to lessen stress on the shoulder.
In freestyle, pain may be felt when the stroke starts because the shoulder is rotated inward when the arm starts pulling through the water. If you’re feeling pain, either decrease the rotation to that side or pull more in front of you (not as wide). This can be a common problem on a swimmer’s non-breathing side because many swimmers lean on that side when they breathe. Make sure not to take the arm across the midline at the start of the stroke as this also can create shoulder impingement issues. Lessening the force of pull at the very start of the freestyle stroke can also lessen the chance of shoulder impingement.
Another biomechanical flaw commonly seen in freestylers occurs at the start of the recovery phase. If pain is felt early in the recovery phase the swimmer might be exaggerating the finish motion too much, and the hand and arm are too high when the recovery starts. Keep the arm lower to the water to start the recovery.
In backstroke, many swimmers press down with their hand and arm to start the stroke. This can definitely make the arm cross behind the back. If you’re feeling pain, either rotate more to that side or aim for a shallower pull.
In butterfly pain may develop when the swimmer presses deep with their chest and the hands stay high at the surface. If you feel pain, press forward with the chest and aim for a flatter stroke.
General Injury Prevention Strategies: ensuring correct technique, core strengthening, mixing strokes during training, adequate rest, strengthening the rotator cuff muscle group, strengthening scapular stabiliser musculature, maintaining equivalent amounts of internal and external rotation around the shoulder, learning to bilateral breath, and carrying out neck and low back flexibility exercises can lessen injury rate in swimmers.
Swimming is enjoyed by both young athletes and older age groups. The more recent popularity of triathlons and adventure sports has encouraged the older athlete to extend their "career" in the discipline of swimming. Most swimming injuries are classed as overuse injuries and relate to faulty biomechanics. Swimming has a distinct profile of injuries. Common problems seen among swimmers include "swimmer's shoulder", an overuse injury that causes inflammation of the supraspinatus tendon, sub-acromial bursa, and/or the biceps tendon, overuse injuries of the elbow (golfer's / tennis elbow), knee injuries (including breastroker's knee), ankle injuries (often tenosynovitis / tendinitis), and back injuries (stress fracture / degenerative).
Common injuries in swimmers include:-
Neck pain: more commonly seen in the older athlete, neck pain is often due to facet joint arthritic change, and disc degeneration +/- nerve root irritation. Muscle innervation and sensation to the shoulder region is predominantly derived from the C5/C6 nerve roots. If these nerve root are irritated due to degenerative change in the neck, shoulder complaints can arise. Arthritic change may also limit neck rotation making correct breathing patterns difficult. Swimmers who do not bilateral breath are more prone to neck pain. Looking forward rather than directly downward, and lifting the head too high when taking a breath can increase load on the neck and create pain.
Swimmer's Shoulder: shoulder injuries are the most common injuries seen in swimmers. "Swimmer's shoulder" is a chronic condition involving repetitive impingement of soft tissue under the coraco-acromial arch. Poor technique plays a huge role in this condition which can lead to sub-acromial bursitis, rotator cuff pathology, and long head of biceps irritation. Other shoulder problems in swimmers often relate to instability of the shoulder due to joint capsule laxity and labral (gleno-humeral gasket) damage, caused by repetitive forces placed on the anterior structures of the shoulder joint.
Breastroker's knee: this overuse condition often seen in breastrokers, involves sprain to the medial collateral ligament (MCL) due to repetitive rotatory / valgus force applied to the knee during the breastroke kick action. Poor technique is implicated in this condition.
Low Back Pain: Hyperextension of the lumbar spine during freestyle and butterfly can create low back pain, as can poor kick technique. In the younger athlete stress fractures are more common, whereas in the older athlete discal degeneration and facet joint degeneration are more common.
Biomechanical flaws: Shoulder Injury Prevention
There are a number of biomechanical flaws in a swimming stroke action which can lead to shoulder pain. Below are some of the more common shoulder issues associated with poor technique, and ways to alter your technique to lessen your chance of injury.
If pain is felt at the beginning of the freestyle stroke or as the arm starts pulling through, this may be due to the upper-arm being positioned behind the back (from shoulder to shoulder): this can cause pain. Swimmers need to be aware their arm position at the start of the stroke: the upper-arm and back have to line up to lessen stress on the shoulder.
In freestyle, pain may be felt when the stroke starts because the shoulder is rotated inward when the arm starts pulling through the water. If you’re feeling pain, either decrease the rotation to that side or pull more in front of you (not as wide). This can be a common problem on a swimmer’s non-breathing side because many swimmers lean on that side when they breathe. Make sure not to take the arm across the midline at the start of the stroke as this also can create shoulder impingement issues. Lessening the force of pull at the very start of the freestyle stroke can also lessen the chance of shoulder impingement.
Another biomechanical flaw commonly seen in freestylers occurs at the start of the recovery phase. If pain is felt early in the recovery phase the swimmer might be exaggerating the finish motion too much, and the hand and arm are too high when the recovery starts. Keep the arm lower to the water to start the recovery.
In backstroke, many swimmers press down with their hand and arm to start the stroke. This can definitely make the arm cross behind the back. If you’re feeling pain, either rotate more to that side or aim for a shallower pull.
In butterfly pain may develop when the swimmer presses deep with their chest and the hands stay high at the surface. If you feel pain, press forward with the chest and aim for a flatter stroke.
General Injury Prevention Strategies: ensuring correct technique, core strengthening, mixing strokes during training, adequate rest, strengthening the rotator cuff muscle group, strengthening scapular stabiliser musculature, maintaining equivalent amounts of internal and external rotation around the shoulder, learning to bilateral breath, and carrying out neck and low back flexibility exercises can lessen injury rate in swimmers.
 Road Cycling Injuries
Road Cycling Injuries
Cycling (Road) Injuries: Ben is a mad keen cyclist and has ridden over 50,000kms locally in and around Dunsborough. That's 9 million revolutions! If you are suffering from a cycling injury Ben is able to help.
Proper frame selection and adjustment can be made by following simple guidelines for frame size, seat height, fore and aft saddle position, saddle angle, reach and handlebar height. Dunsborough Physiotherapy Centre offer a bike-fitting service using formulae, measurement, and observation to get you in an appropriate "fit-zone". The human body functions most effectively in a narrow range of pedal resistance to effort. Increased pedal resistance is a major cause of overuse problems in cyclists: lower gear ratios at a higher cadence is recommended. Over half of traumatic injuries involve motor vehicles, and road surface and mechanical problems with the bicycle are also common causes of accidents. Head injuries are common in cyclists, victims rarely wearing helmets. Contusions, sprains and fractures may occur throughout the body, most commonly involving the hand, wrist, lower arm, shoulder, ankle and lower leg. The handlebar and seat are implicated in a wide variety of abdominal and genital injuries. Abrasions, lacerations and bruises of the skin are the most common traumatic injuries.
Common chronic injuries: chronic (overuse) injuries in road cycling include Guyon's canal syndrome (compression and irritation of the ulnar nerve due to constant pressure applied through the palm of the hand), carpal tunnel syndrome (compression and irritation of the median nerve in the carpal tunnel of the wrist) , trochanteric bursitis (due to iliotibial band tightness / instability of the pelvis on the saddle), low back pain (often sacro-iliac or discal in origin), neck pain (due to sustained cervical extension required when cycling), ilio-tibial band friction syndrome (frictioning of the ITB occurring at the outer side of the knee), patellofemoral syndrome (pain behind the knee-cap due to patella mal-tracking / increased patello-femoral compression), Achilles tendinitis (degeneration of the Achilles tendon), plantar fasciitis (degeneration of the plantar fascia at the site where it attaches into the heel bone under the foot) and Morton's neuralgia (compression and irritation of nerves situated between the metatarsals, leading to pain and altered feeling in the forefoot and toes).
Injury Prevention: trauma may be prevented or reduced by the use of proper protective safety equipment and by maintaining the bike in top mechanical condition. Anticipation of the errors of others and adopting specific riding strategies help to prevent traumatic injuries. Management of overuse injuries in cycling generally involves mechanical adjustment as well as medical management. Neck and back pain are extremely common in cyclists, occurring in up to 60% of riders: better position on the bike can lessen the amount of cervical extension required which is a common cause of neck pain. Making sure you are not too "stretched out" can lessen load on the back walls of the lower discs and the sacro-iliac joint. Strengthening deep neck flexors and scapular retractors can also lessen neck problems. Ulnar neuropathy (Guyon's canal syndrome) characterised by tingling, numbness and weakness in the 4th and 5th digits is common in those riding frequently, as is carpal tunnel syndrome affecting the thumb, 2nd, 3rd and half of the 4th digit. Better hand position on the bars, adequate padding, and lighter grip can alleviate these conditions. Managing saddle-related conditions may involve adjusting seat height, angle, and fore and aft position in addition to changing the saddle. Padding in the saddle and shorts play an important part in saddle problems. Saddle-related problems include chafing, pudendal neuropathy, male impotence, traumatic urethritis and a variety of vulva trauma. Appropriate seat height and fore / aft position can lessen retropatellar compression: the more compression the greater the chance of knee-cap related pain. Calf stretching and strengthening, along with orthotic use can lessen Achilles tendinitis and plantar fasciitis incidence. ITB stretching and gluteal strengthening along with seat height adjustment can lessen the chance of hip bursitis. Appropriate footwear and cleat position can alleviate Morton's neuralgia.
Proper frame selection and adjustment can be made by following simple guidelines for frame size, seat height, fore and aft saddle position, saddle angle, reach and handlebar height. Dunsborough Physiotherapy Centre offer a bike-fitting service using formulae, measurement, and observation to get you in an appropriate "fit-zone". The human body functions most effectively in a narrow range of pedal resistance to effort. Increased pedal resistance is a major cause of overuse problems in cyclists: lower gear ratios at a higher cadence is recommended. Over half of traumatic injuries involve motor vehicles, and road surface and mechanical problems with the bicycle are also common causes of accidents. Head injuries are common in cyclists, victims rarely wearing helmets. Contusions, sprains and fractures may occur throughout the body, most commonly involving the hand, wrist, lower arm, shoulder, ankle and lower leg. The handlebar and seat are implicated in a wide variety of abdominal and genital injuries. Abrasions, lacerations and bruises of the skin are the most common traumatic injuries.
Common chronic injuries: chronic (overuse) injuries in road cycling include Guyon's canal syndrome (compression and irritation of the ulnar nerve due to constant pressure applied through the palm of the hand), carpal tunnel syndrome (compression and irritation of the median nerve in the carpal tunnel of the wrist) , trochanteric bursitis (due to iliotibial band tightness / instability of the pelvis on the saddle), low back pain (often sacro-iliac or discal in origin), neck pain (due to sustained cervical extension required when cycling), ilio-tibial band friction syndrome (frictioning of the ITB occurring at the outer side of the knee), patellofemoral syndrome (pain behind the knee-cap due to patella mal-tracking / increased patello-femoral compression), Achilles tendinitis (degeneration of the Achilles tendon), plantar fasciitis (degeneration of the plantar fascia at the site where it attaches into the heel bone under the foot) and Morton's neuralgia (compression and irritation of nerves situated between the metatarsals, leading to pain and altered feeling in the forefoot and toes).
Injury Prevention: trauma may be prevented or reduced by the use of proper protective safety equipment and by maintaining the bike in top mechanical condition. Anticipation of the errors of others and adopting specific riding strategies help to prevent traumatic injuries. Management of overuse injuries in cycling generally involves mechanical adjustment as well as medical management. Neck and back pain are extremely common in cyclists, occurring in up to 60% of riders: better position on the bike can lessen the amount of cervical extension required which is a common cause of neck pain. Making sure you are not too "stretched out" can lessen load on the back walls of the lower discs and the sacro-iliac joint. Strengthening deep neck flexors and scapular retractors can also lessen neck problems. Ulnar neuropathy (Guyon's canal syndrome) characterised by tingling, numbness and weakness in the 4th and 5th digits is common in those riding frequently, as is carpal tunnel syndrome affecting the thumb, 2nd, 3rd and half of the 4th digit. Better hand position on the bars, adequate padding, and lighter grip can alleviate these conditions. Managing saddle-related conditions may involve adjusting seat height, angle, and fore and aft position in addition to changing the saddle. Padding in the saddle and shorts play an important part in saddle problems. Saddle-related problems include chafing, pudendal neuropathy, male impotence, traumatic urethritis and a variety of vulva trauma. Appropriate seat height and fore / aft position can lessen retropatellar compression: the more compression the greater the chance of knee-cap related pain. Calf stretching and strengthening, along with orthotic use can lessen Achilles tendinitis and plantar fasciitis incidence. ITB stretching and gluteal strengthening along with seat height adjustment can lessen the chance of hip bursitis. Appropriate footwear and cleat position can alleviate Morton's neuralgia.
 Mountain Biking Injuries
Mountain Biking Injuries
Mountain Biking Injuries
Injury rates: 0.37 riders will incur an injury per 100 hours of cross country mountain biking and 4.34 riders per 100 hours of downhill racing. More serious injuries to the head and neck occur whilst falling over the handlebars rather than falling off the bike to the side, which tends to result in lower limb injuries. As a consequence of this, female riders (who are lighter) fall over the handlebars more readily than males, and tend to be more seriously injured than male riders. Most injuries sustained mountain biking occur to young males aged 20–39 years.
Risk factors of injury in mountain bikers are: loss of control, high-speed descending, competitive activity, turning, loss of traction, and mechanical problems. The most common injuries (60–75%) are soft-tissue abrasions, lacerations and contusions. The most prevalent fracture is a clavicular fracture and the most common dislocation affects the acromio-clavicular joint. Concussion is also a common side-effect of a fall off a mountain bike. Neck and back pain are common in mountain bikers: stretching and core strengthening / deep neck flexor strengthening can help to lessen back and neck symptoms. Median nerve irritation at the wrist (carpal tunnel syndrome) and ulnar nerve irritation in the palm (Guyon's canal syndrome) are common in mountain bikers. Padded gloves, lessened grip force and appropriate hand position on the handlebars help to lessen these injuries. Retropatellar pain is common in mountain bike riders: this may result from having the saddle too far forward or too low. In this condition knee pain is felt at the front of the knee- there may be swelling and tenderness around the knee-cap. Metatarsalgia, Morton's neuralgia, achilles tendinitis and plantar fasciitis are common and may all result from incorrect foot position. Foot pain, back of heel pain or under-surface of heel pain may be felt when you press down. Stretching and strengthening of calf musculature, stretching of the plantar fascia, increasing range of motion in the 1st MTP joint, along with a proper bike-fit can help to alleviate these problems.
Injury Prevention: as with road cycling appropriate clothing / protective equipment is essential. Accurate bike-fitting lessens the chance of long-term injury. Getting to know an area before pushing the limits is also important. Racing another cyclist can lead to disaster: remember to take it easy if you are new to mountain biking, or don't know a track well. See Cycling (Road) Injury Prevention for more detailed injury management strategies.
Injury rates: 0.37 riders will incur an injury per 100 hours of cross country mountain biking and 4.34 riders per 100 hours of downhill racing. More serious injuries to the head and neck occur whilst falling over the handlebars rather than falling off the bike to the side, which tends to result in lower limb injuries. As a consequence of this, female riders (who are lighter) fall over the handlebars more readily than males, and tend to be more seriously injured than male riders. Most injuries sustained mountain biking occur to young males aged 20–39 years.
Risk factors of injury in mountain bikers are: loss of control, high-speed descending, competitive activity, turning, loss of traction, and mechanical problems. The most common injuries (60–75%) are soft-tissue abrasions, lacerations and contusions. The most prevalent fracture is a clavicular fracture and the most common dislocation affects the acromio-clavicular joint. Concussion is also a common side-effect of a fall off a mountain bike. Neck and back pain are common in mountain bikers: stretching and core strengthening / deep neck flexor strengthening can help to lessen back and neck symptoms. Median nerve irritation at the wrist (carpal tunnel syndrome) and ulnar nerve irritation in the palm (Guyon's canal syndrome) are common in mountain bikers. Padded gloves, lessened grip force and appropriate hand position on the handlebars help to lessen these injuries. Retropatellar pain is common in mountain bike riders: this may result from having the saddle too far forward or too low. In this condition knee pain is felt at the front of the knee- there may be swelling and tenderness around the knee-cap. Metatarsalgia, Morton's neuralgia, achilles tendinitis and plantar fasciitis are common and may all result from incorrect foot position. Foot pain, back of heel pain or under-surface of heel pain may be felt when you press down. Stretching and strengthening of calf musculature, stretching of the plantar fascia, increasing range of motion in the 1st MTP joint, along with a proper bike-fit can help to alleviate these problems.
Injury Prevention: as with road cycling appropriate clothing / protective equipment is essential. Accurate bike-fitting lessens the chance of long-term injury. Getting to know an area before pushing the limits is also important. Racing another cyclist can lead to disaster: remember to take it easy if you are new to mountain biking, or don't know a track well. See Cycling (Road) Injury Prevention for more detailed injury management strategies.
Triathlon Injuries
Triathlon, Duathlon and Ironman events have become hugely popular in recent years. Due to the large amount of training required to prepare adequately for these events injuries are not uncommon. Injuries often seen in triathlon are covered under Swimming, Cycling, and Running sections above.
Golf Injuries
 Golf Injuries
Golf Injuries
The average golfer typically plays approximately 37 rounds of golf per year. One study has shown that during a two year period, 60% of golf professionals and 40% of amateurs suffered either a traumatic, or overuse injury while playing golf. Over 80 percent of the reported injuries were related to overuse. Low back pain is the most common complaint among both professional and amateur golfers, followed by injuries to the upper extremities (elbow and shoulder). Professional golfers experience a higher number of wrist injuries, and amateur golfers experience more elbow problems. Both groups have a relatively high rate of shoulder injuries.
Low back problems can occur as a result of the powerful rotation and extension motion in the golf swing. In elite golfers the golf swing can generate club head speeds of over 190km/h. Increasing the range of motion of lumbar spine extension and rotation of the lead hip (left hip in right-handed golfers) may decrease the incidence of low back pain. Golfers who carry their own bag have twice the incidence of back, shoulder and ankle injuries as compared with those who do not carry their bag. The elbow is the second most commonly injured area in golfers, and the most common area to suffer from chronic injury. The two most common problems are medial epicondylitis (also known as golfer’s or thrower’s elbow) and lateral epicondylitis (more commonly known as tennis elbow). Both are thought to occur as a result of poor swing mechanics. Medial epicondylitis is thought to be caused by hitting shots “fat” (that is, hitting the ground first), and lateral epicondylitis may be caused by over-swinging with the right hand in right-handed golfers. Both of these problems increase with age and frequency of play. The shoulder is another commonly injured area in golf. Muscles in the shoulder that are most active during the swing are the subscapularis (a rotator cuff muscle), pectoralis major, and latissimus dorsi. Glenohumeral impingement syndrome (bursitis / rotator cuff tendinopathy in the shoulder) and arthritis are the most common shoulder problems seen in golf. These occur most frequently in the lead arm.
Injury Prevention: Good pre-round stretching of the upper extremity and a good strengthening program have been shown to decrease both elbow and shoulder injuries. Those golfers who adequately warm up have less than half the incidence of injuries than those who do not warm up before playing. Good swing biomechanics leads to a lessened injury rate: seek lessens from a golf-pro. Taking as little as 10 degrees off your back swing reduces the incidence of low back pain significantly. A regular exercise program that includes core strengthening, stretching and strengthening of all the major muscle groups used in golf can help decrease your injury rate.
Low back problems can occur as a result of the powerful rotation and extension motion in the golf swing. In elite golfers the golf swing can generate club head speeds of over 190km/h. Increasing the range of motion of lumbar spine extension and rotation of the lead hip (left hip in right-handed golfers) may decrease the incidence of low back pain. Golfers who carry their own bag have twice the incidence of back, shoulder and ankle injuries as compared with those who do not carry their bag. The elbow is the second most commonly injured area in golfers, and the most common area to suffer from chronic injury. The two most common problems are medial epicondylitis (also known as golfer’s or thrower’s elbow) and lateral epicondylitis (more commonly known as tennis elbow). Both are thought to occur as a result of poor swing mechanics. Medial epicondylitis is thought to be caused by hitting shots “fat” (that is, hitting the ground first), and lateral epicondylitis may be caused by over-swinging with the right hand in right-handed golfers. Both of these problems increase with age and frequency of play. The shoulder is another commonly injured area in golf. Muscles in the shoulder that are most active during the swing are the subscapularis (a rotator cuff muscle), pectoralis major, and latissimus dorsi. Glenohumeral impingement syndrome (bursitis / rotator cuff tendinopathy in the shoulder) and arthritis are the most common shoulder problems seen in golf. These occur most frequently in the lead arm.
Injury Prevention: Good pre-round stretching of the upper extremity and a good strengthening program have been shown to decrease both elbow and shoulder injuries. Those golfers who adequately warm up have less than half the incidence of injuries than those who do not warm up before playing. Good swing biomechanics leads to a lessened injury rate: seek lessens from a golf-pro. Taking as little as 10 degrees off your back swing reduces the incidence of low back pain significantly. A regular exercise program that includes core strengthening, stretching and strengthening of all the major muscle groups used in golf can help decrease your injury rate.
Proudly powered by Weebly